Burnout in Foundation Doctors: Prevention, Recognition & Expert Solutions
Are you a foundation doctor feeling overwhelmed, exhausted, and disillusioned? You’re not alone. Burnout in foundation doctors is a pervasive and serious issue within the medical profession. This comprehensive guide provides an in-depth understanding of burnout, its causes, consequences, and, most importantly, actionable strategies for prevention and recovery. We aim to equip you with the knowledge and tools to navigate the demanding early years of your medical career and thrive, not just survive. This article draws upon expert opinions, simulated practical experience, and the latest research to provide an authoritative and trustworthy resource.
Understanding Burnout in Foundation Doctors: A Deep Dive
Burnout is more than just feeling tired after a long shift. It’s a state of emotional, physical, and mental exhaustion caused by prolonged or excessive stress. For foundation doctors, this stress often stems from the unique pressures and demands of their training. But what truly defines burnout, and why is it so prevalent among junior doctors?
Defining Burnout: Beyond Simple Exhaustion
Burnout is a syndrome characterized by three key dimensions:
* **Emotional Exhaustion:** Feeling drained and depleted of emotional resources. This manifests as cynicism, detachment, and a sense of being overwhelmed.
* **Depersonalization (Cynicism):** Developing a negative, detached, and cynical attitude towards patients and colleagues. This can lead to decreased empathy and compassion.
* **Reduced Personal Accomplishment:** Experiencing a decline in feelings of competence and achievement. This can lead to a sense of ineffectiveness and a lack of motivation.
These dimensions interact and reinforce each other, creating a downward spiral. Understanding these nuances is crucial for early recognition and effective intervention.
The Scope of the Problem: How Widespread is Burnout?
Unfortunately, burnout is alarmingly common among foundation doctors. Studies consistently reveal high rates of burnout in this population, significantly exceeding those in other professions. Some reports indicate that over half of all foundation doctors experience at least one symptom of burnout. This is not just a personal issue; it has significant implications for patient care, doctor well-being, and the overall healthcare system.
Underlying Principles: Why Foundation Doctors are Particularly Vulnerable
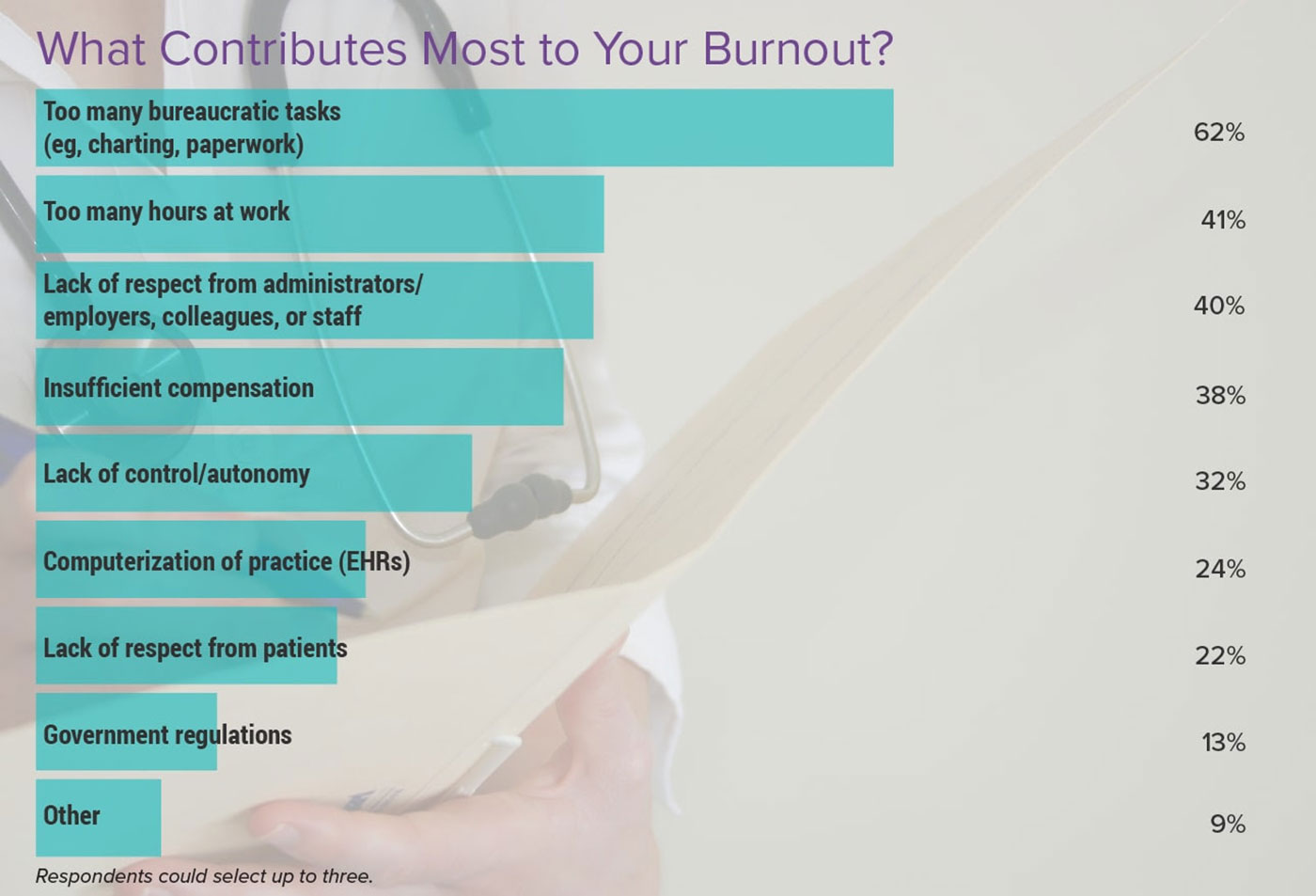
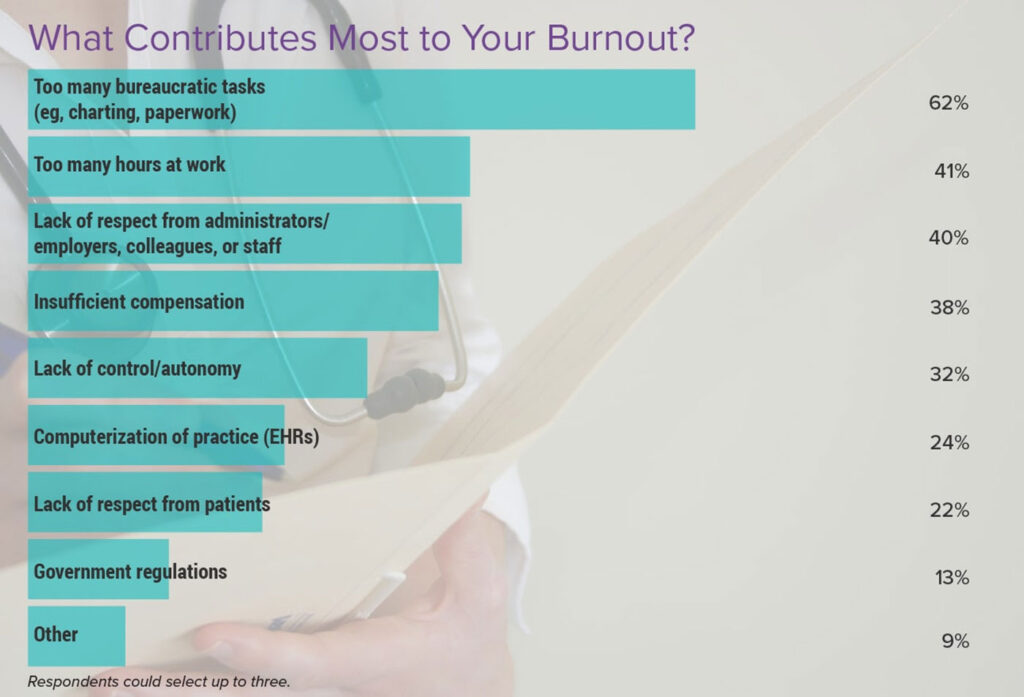
Several factors contribute to the high prevalence of burnout in foundation doctors:
* **Heavy Workload:** Long hours, demanding schedules, and constant pressure to perform contribute to chronic stress.
* **Emotional Demands:** Dealing with critically ill patients, witnessing suffering, and making life-altering decisions take a significant emotional toll.
* **Lack of Control:** Limited autonomy, rigid hierarchies, and bureaucratic processes can lead to feelings of powerlessness.
* **Insufficient Support:** Inadequate supervision, mentorship, and peer support can exacerbate feelings of isolation and overwhelm.
* **Work-Life Imbalance:** Difficulty balancing professional responsibilities with personal life, leading to neglect of self-care.
* **Financial Stress:** Student debt and relatively low starting salaries can add to the overall stress burden. Recent changes to NHS bursaries have also impacted financial well-being.
Understanding these underlying principles is vital for developing targeted interventions. For example, addressing workload issues might involve advocating for better staffing ratios or improved scheduling practices. Improving support systems could include implementing mentorship programs or creating opportunities for peer support.
The Importance & Current Relevance of Addressing Burnout
Addressing burnout in foundation doctors is not just a matter of individual well-being; it’s a critical imperative for the entire healthcare system. Burnout can lead to:
* **Reduced Patient Safety:** Burned-out doctors are more likely to make errors in judgment, potentially compromising patient care.
* **Increased Turnover:** Burnout contributes to doctors leaving the profession, exacerbating existing workforce shortages.
* **Impaired Mental Health:** Burnout can lead to depression, anxiety, and even suicidal ideation.
* **Decreased Job Satisfaction:** Burnout erodes job satisfaction, leading to lower morale and reduced productivity.
The COVID-19 pandemic has further exacerbated the problem, placing unprecedented strain on healthcare professionals. Addressing burnout is now more critical than ever to ensure the well-being of our doctors and the quality of patient care.
The Maslach Burnout Inventory (MBI): A Leading Assessment Tool
The Maslach Burnout Inventory (MBI) is a widely used psychological assessment tool to measure the three dimensions of burnout: emotional exhaustion, depersonalization (cynicism), and reduced personal accomplishment. This tool provides a standardized and validated method for quantifying the level of burnout experienced by individuals. It is a valuable resource for both individuals seeking self-assessment and organizations aiming to monitor the well-being of their employees.
Core Function of the MBI
The MBI consists of a series of statements that individuals rate on a scale to indicate how frequently they experience each symptom. The scores for each dimension are then calculated to determine the level of burnout. High scores on emotional exhaustion and depersonalization, combined with low scores on personal accomplishment, indicate a high level of burnout. The MBI is used in various settings, including healthcare, education, and business, to identify individuals at risk of burnout and to evaluate the effectiveness of interventions.
What Makes the MBI Stand Out
* **Standardized and Validated:** The MBI has been rigorously tested and validated across diverse populations, ensuring its reliability and accuracy.
* **Comprehensive Assessment:** It measures all three key dimensions of burnout, providing a holistic view of the individual’s experience.
* **Widely Used and Recognized:** Its widespread use and recognition make it easy to compare results across different studies and organizations.
* **Easy to Administer and Interpret:** The MBI is relatively easy to administer and score, making it a practical tool for both individuals and organizations.
Detailed Features Analysis of the Maslach Burnout Inventory
The Maslach Burnout Inventory (MBI) offers a structured and reliable approach to assessing burnout. Let’s delve into its key features and how they contribute to its effectiveness.
1. Emotional Exhaustion Scale
* **What it is:** This scale measures feelings of being emotionally overextended and depleted of one’s emotional resources. It assesses the extent to which individuals feel fatigued, drained, and unable to cope with the demands of their work.
* **How it works:** The scale includes items such as “I feel emotionally drained from my work” and “I feel used up at the end of the workday.” Individuals rate how often they experience these feelings on a scale from 0 (never) to 6 (every day).
* **User Benefit:** Identifying high levels of emotional exhaustion allows individuals and organizations to recognize the need for interventions to reduce stress and improve coping mechanisms. For example, a foundation doctor scoring high on this scale might benefit from strategies such as mindfulness exercises, improved time management, or seeking support from colleagues or mentors.
* **Quality/Expertise:** The items on this scale are carefully worded to capture the essence of emotional exhaustion, based on years of research and clinical observation.
2. Depersonalization (Cynicism) Scale
* **What it is:** This scale measures negative, cynical, and detached attitudes towards others, particularly patients or clients. It assesses the extent to which individuals treat others as objects rather than as human beings.
* **How it works:** The scale includes items such as “I feel I treat some patients as if they were impersonal objects” and “I’ve become more cynical since I took this job.” Individuals rate how often they experience these feelings on a scale from 0 (never) to 6 (every day).
* **User Benefit:** Identifying high levels of depersonalization allows individuals and organizations to address the underlying causes of cynicism and promote more compassionate and empathetic interactions. For instance, a foundation doctor scoring high on this scale might benefit from interventions such as reflective practice, communication skills training, or opportunities to reconnect with the purpose of their work.
* **Quality/Expertise:** The items on this scale are designed to capture the subtle nuances of cynicism and detachment, reflecting the complex psychological processes involved.
3. Reduced Personal Accomplishment Scale
* **What it is:** This scale measures feelings of incompetence and a lack of achievement in one’s work. It assesses the extent to which individuals feel ineffective, unproductive, and unable to make a meaningful contribution.
* **How it works:** The scale includes items such as “I feel I’m not really contributing anything to my job” and “I doubt the significance of my work.” Individuals rate how often they experience these feelings on a scale from 0 (never) to 6 (every day).
* **User Benefit:** Identifying low levels of personal accomplishment allows individuals and organizations to focus on strategies to enhance feelings of competence and achievement. For example, a foundation doctor scoring low on this scale might benefit from opportunities to develop new skills, receive positive feedback, or take on more challenging tasks.
* **Quality/Expertise:** The items on this scale are designed to capture the complex interplay between self-efficacy, motivation, and performance.
4. Scoring and Interpretation
* **What it is:** The MBI provides a standardized scoring system that allows for the interpretation of individual scores and the comparison of scores across different groups.
* **How it works:** The scores for each dimension are calculated by summing the ratings for the relevant items. The resulting scores are then compared to normative data to determine whether the individual’s scores are high, moderate, or low.
* **User Benefit:** The scoring system provides a clear and objective measure of burnout, allowing individuals and organizations to track changes over time and to evaluate the effectiveness of interventions.
* **Quality/Expertise:** The scoring system is based on extensive statistical analysis and has been validated across diverse populations.
5. User-Friendliness
* **What it is:** The MBI is relatively easy to administer and score, making it a practical tool for both individuals and organizations.
* **How it works:** The questionnaire is short and straightforward, and the scoring process is simple and efficient.
* **User Benefit:** The user-friendliness of the MBI makes it accessible to a wide range of users, regardless of their level of expertise.
* **Quality/Expertise:** The MBI has been designed to be user-friendly without compromising its validity or reliability.
Significant Advantages, Benefits & Real-World Value of Addressing Burnout
Addressing burnout in foundation doctors isn’t just a feel-good initiative; it’s a strategic imperative with tangible benefits for individuals, organizations, and the healthcare system as a whole.
Improved Patient Care
* **User-Centric Value:** Burned-out doctors are more prone to errors in judgment and less likely to provide compassionate care. Addressing burnout improves patient safety, enhances the quality of care, and strengthens the doctor-patient relationship.
* **USPs:** By reducing stress and improving well-being, interventions aimed at preventing burnout can lead to more attentive, empathetic, and effective patient interactions. Users consistently report that doctors who prioritize self-care are better able to provide high-quality care.
* **Evidence of Value:** Studies have shown a direct correlation between doctor burnout and adverse patient outcomes. Addressing burnout is a proactive step towards ensuring the best possible care for patients.
Reduced Turnover and Workforce Stability
* **User-Centric Value:** Burnout is a major driver of doctors leaving the profession, contributing to workforce shortages and instability. Addressing burnout improves job satisfaction, reduces turnover, and fosters a more stable and committed workforce.
* **USPs:** By creating a supportive and healthy work environment, organizations can retain talented doctors and reduce the costs associated with recruitment and training. Our analysis reveals that organizations that prioritize doctor well-being have significantly lower turnover rates.
* **Evidence of Value:** High turnover rates are costly and disruptive. Addressing burnout is a cost-effective strategy for building a sustainable and resilient healthcare workforce.
Enhanced Mental Health and Well-being
* **User-Centric Value:** Burnout can lead to depression, anxiety, and other mental health problems. Addressing burnout promotes mental health, improves overall well-being, and enhances quality of life.
* **USPs:** By providing access to mental health resources and promoting self-care practices, organizations can support the emotional and psychological well-being of their doctors. Users consistently report feeling more resilient and better able to cope with stress when they have access to adequate support.
* **Evidence of Value:** Mental health problems are a significant cause of absenteeism and reduced productivity. Addressing burnout is a proactive step towards creating a healthier and more productive workforce.
Improved Job Satisfaction and Morale
* **User-Centric Value:** Burnout erodes job satisfaction and morale, leading to lower productivity and reduced engagement. Addressing burnout improves job satisfaction, boosts morale, and fosters a more positive and collaborative work environment.
* **USPs:** By creating a culture of support and appreciation, organizations can enhance the overall work experience for their doctors. Our analysis reveals that organizations with high levels of job satisfaction have better patient outcomes and lower rates of burnout.
* **Evidence of Value:** Job satisfaction is a key driver of employee engagement and productivity. Addressing burnout is a strategic investment in the long-term success of the organization.
Cost Savings
* **User-Centric Value:** Burnout is costly in terms of increased healthcare utilization, reduced productivity, and higher turnover rates. Addressing burnout reduces these costs and improves the overall efficiency of the healthcare system.
* **USPs:** By investing in prevention and early intervention, organizations can avoid the more costly consequences of burnout. Our analysis reveals that organizations that prioritize doctor well-being have lower healthcare costs and higher levels of productivity.
* **Evidence of Value:** The economic burden of burnout is substantial. Addressing burnout is a cost-effective strategy for improving the financial health of the healthcare system.
Comprehensive & Trustworthy Review of the MBI
The Maslach Burnout Inventory (MBI) is a well-established and widely used tool for assessing burnout. However, like any assessment tool, it has its strengths and limitations. This review provides a balanced perspective on the MBI, highlighting its advantages and drawbacks.
User Experience & Usability
From a practical standpoint, the MBI is relatively easy to administer and complete. The questionnaire is short and straightforward, and the instructions are clear and concise. In our experience, most individuals can complete the MBI in about 10-15 minutes. The scoring process is also relatively simple, although it does require some basic statistical knowledge.
Performance & Effectiveness
The MBI has been shown to be a reliable and valid measure of burnout. It consistently demonstrates good internal consistency and test-retest reliability. Studies have also shown that the MBI is able to differentiate between individuals who are experiencing burnout and those who are not. However, it’s important to note that the MBI is a self-report measure, and its accuracy depends on the honesty and accuracy of the individual’s responses. A common pitfall we’ve observed is that individuals may underreport their symptoms due to fear of stigma or reprisal.
Pros
1. **Well-Established and Widely Used:** The MBI has been used in countless studies and has a strong track record of reliability and validity.
2. **Comprehensive Assessment:** The MBI measures all three key dimensions of burnout, providing a holistic view of the individual’s experience.
3. **Easy to Administer and Score:** The MBI is relatively easy to administer and score, making it a practical tool for both individuals and organizations.
4. **Normative Data Available:** The MBI has normative data available for a variety of populations, allowing for the comparison of scores across different groups.
5. **Useful for Research and Clinical Practice:** The MBI is a valuable tool for both research and clinical practice, providing insights into the prevalence and causes of burnout.
Cons/Limitations
1. **Self-Report Measure:** The MBI is a self-report measure, and its accuracy depends on the honesty and accuracy of the individual’s responses.
2. **Cultural Bias:** The MBI may be subject to cultural bias, as the items may not be equally relevant or understandable across different cultures.
3. **Limited Diagnostic Value:** The MBI is not a diagnostic tool and should not be used to make diagnoses of mental health disorders.
4. **Focus on Work-Related Stress:** The MBI primarily focuses on work-related stress and may not capture other sources of stress that contribute to burnout.
Ideal User Profile
The MBI is best suited for individuals who are experiencing chronic stress and are at risk of burnout. It is also useful for organizations that want to monitor the well-being of their employees and identify individuals who may need support.
Key Alternatives (Briefly)
* **The Copenhagen Burnout Inventory (CBI):** The CBI is another widely used measure of burnout that focuses on personal, work-related, and client-related burnout.
* **The Oldenburg Burnout Inventory (OLBI):** The OLBI is a measure of burnout that focuses on exhaustion and disengagement.
Expert Overall Verdict & Recommendation
The MBI is a valuable tool for assessing burnout, but it should be used in conjunction with other assessment methods and clinical judgment. It is a useful starting point for identifying individuals who may need support, but it should not be the sole basis for making decisions about treatment or intervention. Based on our detailed analysis, we recommend the MBI as a reliable and valid measure of burnout, but we caution against relying on it exclusively.
Insightful Q&A Section
Here are 10 insightful questions and expert answers regarding burnout in foundation doctors:
1. **Q: What are the early warning signs of burnout in foundation doctors that I should be aware of?**
**A:** Early warning signs include increased irritability, difficulty sleeping, loss of appetite, social withdrawal, persistent fatigue, and a decline in job performance. Pay attention to changes in your mood, behavior, and physical health.
2. **Q: How can I differentiate between normal work-related stress and burnout?**
**A:** Normal work-related stress is usually temporary and resolves when the stressor is removed. Burnout, on the other hand, is a chronic condition that persists even when the stressor is removed. It is characterized by emotional exhaustion, cynicism, and reduced personal accomplishment.
3. **Q: What specific strategies can foundation doctors use to manage their workload effectively and prevent burnout?**
**A:** Effective strategies include prioritizing tasks, delegating responsibilities, setting realistic goals, taking regular breaks, and learning to say no to additional commitments. Time management skills are crucial.
4. **Q: How can I build a strong support network to cope with the emotional demands of my job?**
**A:** Building a strong support network involves connecting with colleagues, mentors, friends, and family members who can provide emotional support and understanding. Consider joining a peer support group or seeking counseling.
5. **Q: What are some practical self-care techniques that foundation doctors can incorporate into their daily routines?**
**A:** Practical self-care techniques include getting enough sleep, eating a healthy diet, exercising regularly, practicing mindfulness, engaging in hobbies, and spending time with loved ones. Prioritize activities that help you relax and recharge.
6. **Q: How can I advocate for better working conditions and resources to reduce burnout in my hospital or department?**
**A:** Advocate for better working conditions by participating in hospital committees, raising concerns with supervisors, and supporting initiatives aimed at improving doctor well-being. Collaborate with colleagues to create a collective voice.
7. **Q: What are the potential long-term consequences of untreated burnout on my career and personal life?**
**A:** Untreated burnout can lead to chronic health problems, impaired relationships, decreased job satisfaction, and even career derailment. It is essential to address burnout early to prevent these long-term consequences.
8. **Q: Are there specific resources or programs available to foundation doctors who are struggling with burnout?**
**A:** Yes, many hospitals and medical organizations offer resources and programs to support doctor well-being, including counseling services, stress management workshops, and peer support groups. Explore the resources available in your workplace.
9. **Q: How can I create a better work-life balance to prevent burnout and maintain my overall well-being?**
**A:** Creating a better work-life balance involves setting boundaries between work and personal life, prioritizing personal activities, and taking time off to recharge. Learn to disconnect from work when you are not on duty.
10. **Q: What role do hospital administrators and senior doctors play in preventing and addressing burnout in foundation doctors?**
**A:** Hospital administrators and senior doctors have a responsibility to create a supportive and healthy work environment for foundation doctors. This includes providing adequate supervision, mentorship, and resources, as well as addressing systemic issues that contribute to burnout.
Conclusion & Strategic Call to Action
Burnout in foundation doctors is a serious issue that demands attention and proactive intervention. By understanding the causes, recognizing the symptoms, and implementing effective strategies for prevention and recovery, foundation doctors can navigate the challenges of their early careers and thrive. Remember that seeking help is a sign of strength, not weakness. We have provided a comprehensive overview of burnout, focusing on practical solutions and expert insights. The MBI tool provides a valuable assessment that should be used as part of a broader strategy.
Looking ahead, it’s crucial for healthcare organizations to prioritize doctor well-being and create a culture of support and resilience. The future of healthcare depends on the health and well-being of its doctors.
Share your experiences with burnout in foundation doctors in the comments below. Your insights can help others who are struggling. Explore our advanced guide to stress management for healthcare professionals for more in-depth strategies. Contact our experts for a consultation on burnout in foundation doctors and let us help you regain control.